
The Ragon Institute of Mass General Hospital, MIT, and Harvard has a dual mission to contribute to the accelerated discovery of an HIV/AIDS vaccine and subsequently to establish itself as a world leader in the collaborative study of immunology. Thus, the vast majority of studies require the use of peripheral blood cells such as B and T lymphocytes, monocytes, and neutrophils. Most researchers at the Ragon Institute work with millions of these peripheral blood cells every day—but where do they come from and how do they end up in the lab of a Ragon researcher?
It all starts with a request from a researcher. The week before a researcher needs the cells, she or he must submit a request to Daniel Worrall, ANP-BC, a nurse practitioner specialist at Massachusetts General Hospital (MGH) who directs the blood collection clinic at the Ragon Institute. In this report, the researcher must include the concept sheet for the experiment detailing exactly what she or he intends to do with the blood, what kind of cells she or he needs, the number of subjects, and what kind of subject (e.g. sex, age, ethnicity, HIV+/-) she or he needs. Once the request is in, Worrall will contact study participants to set up appointments to come in and donate blood.
Study participants are recruited via a multitude of advertisements posted on blood donation email lists and posters around the Technology Square area. Most of the subjects who volunteer for studies at the Ragon Institute are actually MGH employees who hear about the studies through the MGH weekly “Research Participants Needed” email. The only financial incentive to donate blood to the Ragon Institute is a $15 stipend (for HIV- study participants) which helps ensure that study participants are fully consenting to the procedure. Ragon Institute employees are firmly banned from enrolling in any Ragon studies.
The studies at the Ragon Institute are longitudinal, so once people get involved in a study they can stay active for up to five years. Healthy volunteers can donate blood as often as they want, up to 550mL of blood within an eight week period. HIV+ subjects can donate up to 200mL of blood in an eight week period. In addition, volunteers must weigh over 110 pounds.
 Studies at the Ragon Institute can be categorized into two overarching groups—studies that investigate immunology in healthy cohorts and studies that investigate immunology in HIV+ cohorts. Subjects enrolled in HIV+ studies have their blood drawn at the main MGH campus in downtown Boston and subjects enrolled in HIV- studies have their blood collected at the Ragon Institute in Technology Square in Cambridge.
Studies at the Ragon Institute can be categorized into two overarching groups—studies that investigate immunology in healthy cohorts and studies that investigate immunology in HIV+ cohorts. Subjects enrolled in HIV+ studies have their blood drawn at the main MGH campus in downtown Boston and subjects enrolled in HIV- studies have their blood collected at the Ragon Institute in Technology Square in Cambridge.
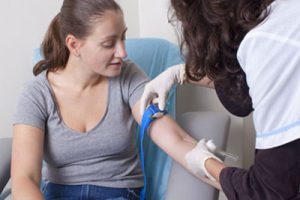
When a subject arrives at the blood collection clinic, they first are asked a series of questions about their health and medical history to make sure it is appropriate for them to donate blood. Some of the questions might be: Has anything changed in your medical history? Have you had surgery since I last saw you? Are you currently taking any medications? Have you had any vaccines since I last saw you? Are you able to get pregnant? Or, are you currently using any contraceptives? This information is then entered into the source document, or case report, for the visit.
After the case report is completed, the patient will sit in a comfortable chair and have 40-60mL of blood drawn. Safety blood labs are drawn annually to screen for hemoglobin efficiency, platelet count, and HIV or hepatitis B/C infection.
After the patient leaves the clinic, all of the data collected in the case report is entered into the Ragon Institute’s Cellular Immunology Database (CIDB). The CIDB is accessible by all Ragon researchers, and contains details about all subjects enrolled in Ragon studies, including case report information, what studies she or he is enrolled in, previous studies she or he has participated in, and who received the blood specimens. The CIDB also keeps track of the concept sheet for every experiment that a subject participates in.
It is important to note that there is no identifying information available on the CIDB and all subjects are identified by a random ID number. In addition, study participants are allowed access to the CIDB to check their profile and the information contained on it at all times.
Once all of the patient information is entered into the CIDB, the researcher who requested the blood sample is notified.
In order to transport blood from the clinic to the researcher, the vacutainers of blood collected in the clinic must first be enclosed in a plastic biohazard bag and then sealed inside a specialized transport vessel. If blood specimens are coming from the MGH main campus to Ragon, they must be secured in an additional vessel for a third layer of protection.
Blood samples are placed in the specimen drop box outside of Ragon Blood Processing Lab, directed by Dr. Ildiko Toth. Researchers can either pick up the fresh blood directly from the drop box or request for the blood to be processed in the Processing Lab for specific types of cells.
If a researcher wishes to perform an experiment on a specific population of cells (lets say, CD4+ T cells for instance) they can request that the Processing Lab isolate these specific cells from the blood. There are many complex protocols which blood processing technicians are extensively trained in to isolate certain types of cells.
For example, isolating CD4+ T cells from a sample of fresh blood necessitates a biosafety level two lab which requires a fluid-resistant lab coat, two pairs of latex exam gloves, eye goggles, and a tissue culture fume hood. In order to separate the CD4+ T cells from the whole blood, the technician must go through a series of precise steps in which they prepare a unique solution of nutrients, antibiotics, and ions to stabilize the sample, transfer the blood from a blood bag or vacutainer to a conical tube, carefully add a layer of high density ficoll to the bottom of the test tube, and go through a series of centrifuge spins, aspirations, and pipette draws.
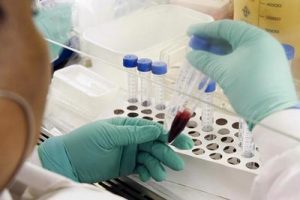 If this laborious process is done correctly, the technician will be left with a purified population of peripheral blood mononuclear cells (PBMCs). To isolate CD4+ T cells from this population, the technician must once again prepare a precise solution of nutrients and then add carefully engineered CD4+ antibodies tagged with microscopic magnets which allow her or him to carefully remove just the CD4+ T cells from the sample using specialized magnets. This sample can then be used right away by the researcher or stored in a cryotube and placed in a liquid nitrogen freezer for later use. Some samples of blood cells at the Ragon Institute are greater than twenty years old.
If this laborious process is done correctly, the technician will be left with a purified population of peripheral blood mononuclear cells (PBMCs). To isolate CD4+ T cells from this population, the technician must once again prepare a precise solution of nutrients and then add carefully engineered CD4+ antibodies tagged with microscopic magnets which allow her or him to carefully remove just the CD4+ T cells from the sample using specialized magnets. This sample can then be used right away by the researcher or stored in a cryotube and placed in a liquid nitrogen freezer for later use. Some samples of blood cells at the Ragon Institute are greater than twenty years old.
In addition to isolating PBMCs, the Ragon Processing Lab also processes all blood donations from the Mass General Hospital Infectious Disease Unit, isolates blood plasma which is crucial to examining proteins found in both HIV positive and negative blood, extracts DNA samples, and manages the CIDB as well as the tens of thousands of cryosamples housed in the Ragon Institute’s vast network of liquid nitrogen freezers.
Researchers at the Ragon Institute and biomedical research institutions across the world use blood cells in their research every day, but we often forget how the cells ended up the lab in the first place. Retrieving one miniscule tube of CD4+ T cells requires the full fledged efforts and coordination of countless personnel in the communications department, blood collection clinic, blood processing lab, research laboratory personnel, and most importantly, our generous blood donors and study participants.
If you would like to support our research by being involved in a study, we are always looking for volunteers, both HIV positive or negative. Contact our Clinical Department and they will discuss your eligibility with you. All personal information about research participants is kept strictly confidential.
Additionally, we encourage you to register with RSVP for Health, a service which provides study participants with a comprehensive list of studies for which they are eligible.
The Ragon Institute does not test or treat those with HIV/AIDS, but we are committed to developing a vaccine for HIV/AIDS. If you are interesting in testing or treatment, we suggest that you contact the Mass General Hospital Infectious Disease Unit.

Liam is a lifelong resident of Boston and is currently enrolled at the University of Massachusetts in Amherst majoring in Biochemistry and Molecular Biology on a pre-medical track. In his freshman year at UMass, Liam was elected the House Council President of the UMass Northeast residential area and was selected as one of fifteen members of the inaugural Biology Major Advisory Committee. Last year, Liam authored and published a book titled Through the Eyes of Our Neighbors which explores the differing identities of Boston as it pertains to people of different racial groups, socioeconomic classes, and nationalities through portraits and interviews collected from over 70 people. This summer, Liam is working full time at the Ragon Institute of Mass General, MIT, and Harvard alongside Sarah Sullivan and Dr. Sylvie Le Gall as a liaison between the research laboratories and communications department. For personal inquiries, email Liam at lsfitzgerald@umass.edu.